|
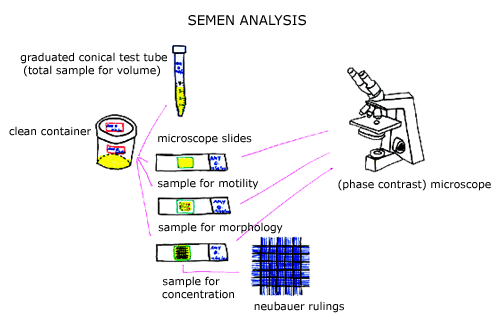
The semen analysis can provide a great deal of information about the functional status of the male reproductive system. In order to produce a normal semen analysis, there must be proper functioning of the male reproductive hormone system, spermatogenesis and spermiogenesis within the testes, and patency of the male outflow tract.
The World Health Organization has a Laboratory Manual for the Examination of Human Semen and Semen Cervical Mucus which I have found to be invaluable in my own training. Three of the major variables examined in the semen analysis include sperm concentration, sperm motility, and sperm morphology (shape).
Counting the number of sperm within a counting chamber assesses sperm concentration. A typical bright line counting chamber will have a ruling pattern (that is very precisely constructed) such as that seen in the Neubauer rulings. In the Neubauer chamber there is a central square millimeter that is ruled into 25 groups of 16 small squares. The concentration of sperm is calculated depending on the volume within each area of the chamber (with the Neubauer chamber the number of cells per mL is the number of cells counted per square millimeter x 10,000 x any dilution factor used).
Looking at a representative sample of the semen under the microscope and calculating the percentage of sperm that are actually moving assess sperm motility. The % motility is 100 x the number of motile sperm divided by the total number of sperm counted.
Sperm morphology is easiest to assess with a bright light microscope after the sperm have been stained. Various stains for cells and tissues are available.
It is important to recognize that a semen analysis is not a sperm function test. A normal semen analysis (with a normal concentration of adequately moving and normal shaped sperm) does not necessarily mean that the sperm is capable of fertilizing an egg (its primary biological function).
|

|